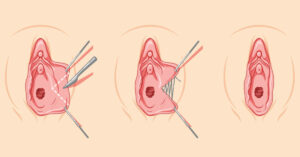
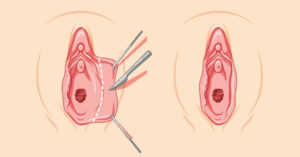
Labiaplasty is a specialized surgical procedure designed to reshape or reduce the labia minora and, in some cases, the labia majora. While many women seek treatment for aesthetic reasons, a significant number pursue surgery due to persistent discomfort, irritation, hygiene challenges, or interference with physical activity. One of the most common and important questions patients ask is whether labiaplasty is covered by insurance.
The answer is nuanced. Insurance coverage depends largely on whether the procedure is considered cosmetic or medically necessary. This comprehensive guide explains how insurers evaluate claims, what documentation is required, and what patients should realistically expect.
Understanding Labiaplasty: Cosmetic vs. Medical Indications
Before determining if labiaplasty is covered by insurance, it is essential to understand how insurers classify the procedure. Labiaplasty is often labeled as elective cosmetic surgery. However, labial hypertrophy can cause legitimate medical concerns1, including:
- Chronic irritation from clothing
- Pain during exercise or cycling
- Discomfort during sexual activity
- Recurrent skin breakdown or infections
- Hygiene difficulties
In such cases, the procedure may move beyond aesthetics. The documented benefits of labiaplasty can include improved physical comfort, reduced inflammation, enhanced hygiene, and restored confidence. When functional impairment is clearly established, the question shifts from purely cosmetic enhancement to medical necessity.
This distinction directly affects whether insurance will cover labiaplasty in your specific case.
How Insurance Companies Define Medical Necessity
Insurance providers rely on strict criteria to determine when labiaplasty is covered by insurance. Most insurers use medical policy guidelines that require:

- Documented functional impairment
- Failure of conservative treatments
- Physical examination findings supporting the complaint
- Photographic documentation in some cases
If symptoms interfere with daily living or physical activity, insurers may consider whether insurance can cover labiaplasty under reconstructive or medically indicated surgery policies.
However, cosmetic dissatisfaction alone typically does not meet the threshold. Therefore, when patients ask if insurance pays for labiaplasty, the honest answer is that it rarely does without strong medical documentation.
Common Scenarios: When Coverage May Be Possible
Although uncommon, there are situations where labiaplasty can be covered by medical insurance. These often include:
- Persistent rashes or ulcerations unresponsive to topical therapy
- Pain that limits exercise or employment duties
- Anatomical abnormalities causing significant functional impairment
- Post-traumatic or post-surgical deformities
In these circumstances, surgeons must carefully document symptoms, duration, failed conservative management, and objective findings. Even then, approval is not guaranteed.
Many women considering surgery want to know what insurance covers labiaplasty, but there is no universal list of carriers that routinely approve the procedure. Coverage depends more on individual policy language than the company itself.
Why Most Insurance Claims Are Denied
To understand whether labiaplasty is covered by insurance, it is equally important to understand why claims are often denied. The most common reasons include:

- Classification as cosmetic surgery
- Lack of documented functional limitation
- Absence of conservative treatment attempts
- Insufficient medical records
Insurers may argue that enlarged labia fall within normal anatomical variation. Because of this, many patients are ultimately responsible for out-of-pocket costs. This reality makes it essential to approach the process strategically if you are exploring how to get labiaplasty covered by insurance.
Step by Step: How to Strengthen a Claim
If you believe your case is medically justified, here are practical steps on how to get labiaplasty covered by insurance:
1. Seek Evaluation from an Experienced Surgeon
Choose a specialist who understands both the functional and anatomical aspects of labial hypertrophy. Detailed documentation is critical.
2. Document Symptoms Thoroughly
Maintain records describing pain, interference with activity, hygiene issues, or recurrent infections.
3. Attempt Conservative Treatment
Insurance companies often require proof that non-surgical options were ineffective.
4. Verify Policy Language
Review your insurance handbook carefully to determine what insurance covers labiaplasty under reconstructive or medically necessary provisions.
5. Submit Preauthorization
Always request preapproval to clarify whether insurance can cover labiaplasty in your specific situation. Even with strong documentation, patients must be prepared for possible denial. This does not necessarily end the process.
The Appeals Process Explained
If your claim is denied, it does not mean the process is over. You still have the right to appeal the decision, and many patients revisit the possibility of insurance coverage during this stage with stronger documentation and additional medical support. An appeal typically requires:

- A detailed letter from your surgeon explaining the medical necessity
- Supporting clinical photographs
- Records of failed conservative treatment
- Peer-reviewed literature supporting functional impairment
Appeals can take weeks or months. While success rates vary, persistence and thorough documentation improve the likelihood that insurance can cover labiaplasty after reconsideration.
Financial Planning if Insurance Does Not Cover It
Because approval is unpredictable, many patients ultimately learn whether insurance pays for labiaplasty in their case. When it does not, alternative options include:
- Healthcare financing programs
- Payment plans
- Health Savings Accounts
- Flexible Spending Accounts
Understanding costs in advance allows you to plan responsibly. While cost matters, choosing an experienced surgeon is critical for safety, optimal outcomes, and minimizing complications.
Surgical Expertise and Medical Evaluation Matter
An often overlooked factor in determining when labiaplasty is covered by insurance is the quality of the medical evaluation. Surgeons with advanced training in vaginal rejuvenation are better equipped to distinguish between cosmetic preference and clinically significant hypertrophy.

They can also explain the surgical approach, expected outcomes, and the full labiaplasty recovery timeline, which typically includes:
- Initial swelling and tenderness for one to two weeks
- Gradual return to exercise after four to six weeks
- Complete tissue healing over several months
Understanding recovery reinforces whether the procedure addresses meaningful functional concerns or primarily aesthetic goals. Patients asking whether labiaplasty can be covered by medical insurance should seek providers who understand insurance criteria as well as surgical precision.
Key Questions to Ask Your Insurance Provider
If you are exploring whether your procedure may qualify for insurance coverage, the most reliable next step is to contact your insurance provider directly and ask the following questions:
- Does my policy exclude cosmetic genital surgery?
- Under what conditions can insurance cover labiaplasty?
- What documentation is required?
- Is preauthorization mandatory?
- Are appeals permitted if initially denied?
Clear communication helps clarify what insurance covers labiaplasty under your specific plan. Each policy differs, so individualized verification is essential.
Setting Realistic Expectations
Despite the desire for coverage, statistics suggest that most patients will find a negative answer to whether labiaplasty is covered by insurance2. Insurance carriers tend to maintain strict cosmetic exclusions.

However, for women experiencing significant pain, irritation, or daily interference, there are circumstances where insurance will cover labiaplasty after a detailed review.
The most important takeaway is this: insurance decisions are based on documentation and policy language, not patient preference alone. If you are exploring how to get labiaplasty covered by insurance, preparation and professional guidance are essential.
Making an Informed, Empowered Decision
Ultimately, whether labiaplasty is covered by insurance depends on medical necessity, policy terms, and supporting evidence. For some patients, insurance may cover labiaplasty when functional impairment is clearly demonstrated. For many others, insurance will not classify the procedure as medically required.
Understanding whether insurance pays for labiaplasty, reviewing what insurance covers labiaplasty, and learning when labiaplasty is covered by insurance allows you to make an informed decision grounded in facts rather than assumptions.
A consultation with a qualified specialist can clarify your anatomical concerns, evaluate medical necessity, and guide you through the next steps, whether insurance approval is possible or not.
Advanced Care and Personalized Surgical Solutions

At Alinea Labiaplasty & Vaginoplasty Michigan, we provide cutting-edge labiaplasty surgery using refined techniques designed for both functional relief and aesthetic precision. If you are seeking clarity about insurance or treatment options, contact our experienced team to schedule a confidential consultation and personalized evaluation.
References
- Johnson, J. (2023, October 25). What is labial hypertrophy and is it normal? https://www.medicalnewstoday.com/articles/322755
- Rowley M, Thawanyarat K, Shah J, Nazerali R. Labiaplasty and Insurance: To Cover or Not to Cover? Arch Plast Surg. 2022 Apr 6;49(2):285-286. doi: 10.1055/s-0042-1744428. PMID: 35832678; PMCID: PMC9045511.